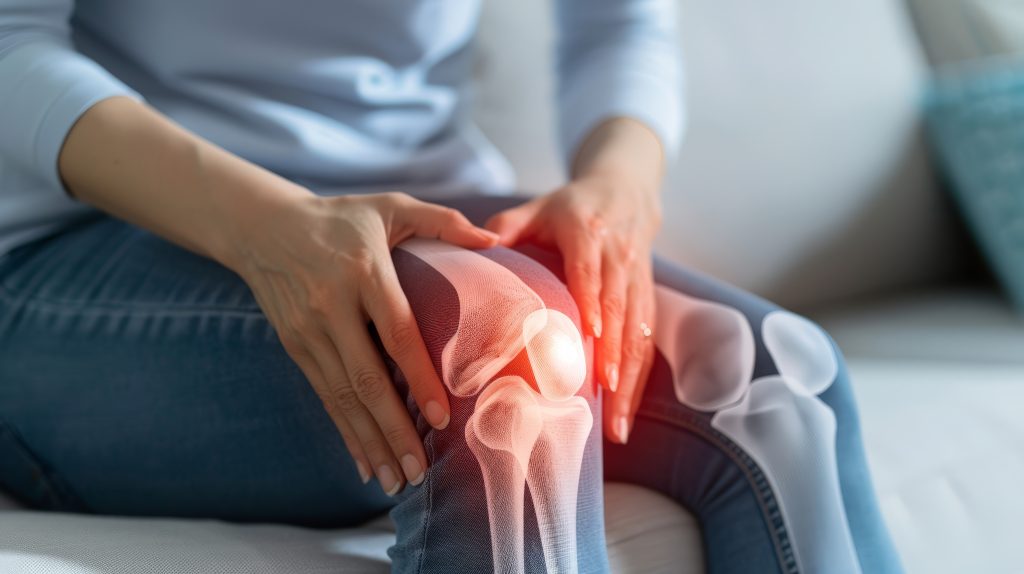
Patellar instability
Patellar instability | Patellar dislocation
Acute care & follow-up treatment
ÜBERSICHT
A basic distinction is made between congenital patellar instability and trauma that has caused the kneecap to dislocate outwards (patellar luxation).
Traumatic patellar dislocations that occur for the first time following a significant trauma can usually be treated conservatively. Surgical treatment is only considered in cases of persistent instability or recurrent dislocations following conservative therapy.
In the case of congenital patellar instability (habitual patellar instability), the anatomy of the entire leg must be analyzed in more detail. There can be a wide variety of causes for instability:
- Protruding kneecap
- Rotational defect of the upper or lower leg
- X-legs
- Maldevelopment of the V-shaped patellar groove (trochlear dysplasia)
- Insufficiency of the patellar support apparatus (medial patellofemoral ligament - MPFL)
Symptoms of patellar instability
With chronic instability of the kneecap, most patients complain of a fundamental fear of a new dislocation (luxation), which can be extremely painful each time. Sports activities can no longer be practiced, even climbing stairs can be problematic.
Unnatural movements lead to chronic incorrect loading of the joint cartilage and thus to early development of joint wear (osteoarthritis). After repeated dislocations of the kneecap, there is often already a high degree of cartilage damage, which must also be treated.
Diagnosis of a patellar dislocation
The first diagnostic step is always a clinical assessment. Particularly in chronic cases, the cause of the instability can be deduced from the instability in different degrees of flexion of the knee joint. The bony anatomy or bony shearing injuries can be identified by means of an X-ray. An X-ray of the entire leg axis can also provide information about an existing malalignment (knock-knee). A magnetic resonance scan is essential to assess the cartilage surface, but also to evaluate the ligament structures and the patellar groove. Only in rare cases of instability with degrees of flexion greater than 60° should a CT scan of the leg also be performed to assess congenital malrotation of the thigh or lower leg.
Treatment options for patellar dislocation
If the kneecap is still in a dislocated state, it should be repositioned as an immediate measure. In the case of a pronounced knee joint effusion, the effusion should be aspirated (punctured). On the one hand, this has a pain-relieving effect, but on the other hand the effusion pushes the kneecap further outwards and is therefore rather counterproductive for conservative therapy.
After an initial patellar dislocation, the risk of another such injury is approximately 30%. Traumatic patellar dislocations that occur for the first time following a significant trauma can usually be treated conservatively. This is contingent on the trauma not having caused significant cartilage damage. Treatment involves immobilizing the knee joint in a straightened position using a splint (orthosis) for about 1–2 weeks. Anschließend wechselt man für weitere 4 Wochen auf eine weichere Bandage (z.B.: Patella Pro Bandage), die die Kniescheibe aktiv nach Innen zieht.
After multiple dislocations of the kneecap, however, surgery should be performed to stabilize the kneecap.
The following operations can be performed:
- MPFL PLASTIC: Tendonplasty of the torn ligament on the inside of the kneecap.
- TUBEROSITAS REPLACEMENT (Elmslie-Trillat operation): Inward displacement of the insertion of the patellar tendon at the tibial plateau is considered in cases of increased patellar elevation.
- TROCHLEADYSPLASIA (malformation of the patellar gliding groove): The sliding groove must be surgically milled out and modeled (TROCHLEAPLASTY)
- AXIAL CORRECTIONS of the thigh